
Values are showed as median (interquartile range), or percentage (n%) We tested the method to use the combined score, which further stratified TIMI medium-risk patients into the GRACE ≥ 140 subgroup and GRACE < 140 subgroups. To explore the optimal risk score in our study population, we examine a way to reserve the two risk scores’ convenience and predictive accuracy. We also used online risk calculators following the recommendation by 2020 ESC guideline. Patients who scored ≤ 108 points were low-risk, 109–139 points were medium-risk, ≥ 140 points were high-risk. GRACE score was calculated on admission based on the following variables: age, heart rate (HR), systolic blood pressure (SBP), initial serum creatine (Cr), Killip classification, cardiac arrest at presentation, initial cardiac enzyme positive, and ST-segment deviation. Patients with 0–2 scores were low-risk groups while 3–4 scores were medium-risk groups and 5–7 scores were high-risk. Patients achieved 1 point for yes and 0 points for no. In UA/NSTEMI, TIMI scores incorporated the following 7 points: age ≥ 65 years, ≥ three coronary artery disease (CAD) risk factors, known coronary stenosis > 50%, aspirin used in the past 7 days, severe angina (≥ 2 episodes w/in 24 h), severe angina (≥ 2 episodes w/in 24 h) and positive cardiac marker. In this observational study, we sought to (1) examine the distribution of risk tertiles by GRACE versus TIMI in a contemporary cohort of NSTEMI East Asian patients in today's reperfusion era, (2) compare the predictive ability between GRACE and TIMI risk score, (3) explore the optimal way for risk stratification in East Asian population by combining these two scores.īoth GRACE and TIMI risk scores were calculated on admission. Nevertheless, limited evidence compared the usefulness of these two major risk scores and their association with both in-hospital events and long-term outcomes in contemporary East Asian patients. Studies proved TIMI’s advantage in its simplicity in clinical application and GRACE's favorable discriminative power. GRACE and TIMI are the two most popular prediction models in ACS developed during the prereperfusion era and have been compared face to face mainly in the Caucasian population. Therefore, there is an essential need to assess individual risk easily and accurately. Guidelines recommend that high-risk patients receive more aggressive invasive treatment upon risk stratification on admission. Risk assessment was crucial in guiding therapeutic decision-making. However, NSTEMI patients have a large range of clinical consequences, from minimal sequelae to early death. 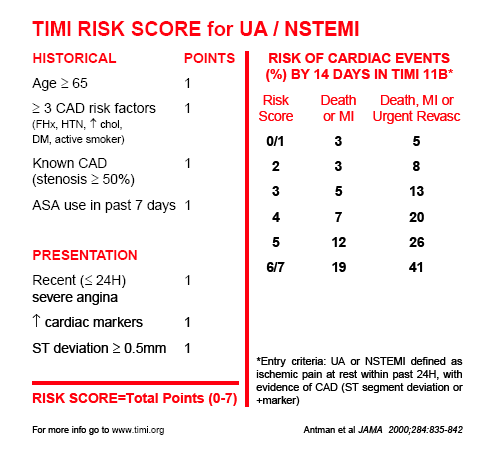
A major component of ACS, Non-ST segment elevation myocardial infarction (NSTEMI), has more than twice the incidence compared to ST-segment elevation myocardial infarction (STEMI). The prevalence of acute coronary syndromes (ACS) has increased significantly during the recent 30 years in China. 
Combined use of the two risk scores reserved both the convenience of scoring and the predictive accuracy.Ĭardiovascular disease remains the main contributor to the cause of death globally. 0.68 long-term cardiac mortality: 0.91 vs. GRACE risk scores showed a better predictive ability than TIMI risk scores both for in-hospital and long-term outcomes. Compared to TIMI medium group + GRACE < 140 subgroup, the TIMI medium + GRACE high-risk (≥ 140) subgroup had a significantly higher in-hospital events (39.5% vs. Further subgrouping the TIMI medium group showed that half (53.5%) of the TIMI medium risk population was GRACE high risk (≥ 140). GRACE score grouped most patients (45.7%) into high risk, while TIMI grouped the majority (61.2%) into medium risk. The Creative Commons Public Domain Dedication waiver ( ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.Ī total of 232 patients were included (female 29.7%, median age 67 years), with a median follow-up of 3.7 years. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. Open AccessThis article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
